Preventing blood clots in pregnant mothers poses significant health care challenges. The risk of blood clots in pregnant mothers is almost ten times more likely than a non-pregnant woman. These patient safety risks increase for pregnant mothers who are obese. In the United States, more than two-thirds of adults are obese. Continue reading “Keeping Pregnant Mothers Safe from Blood Clots: Managing the Health Care Risk in Obese Patients”
Tag: Pat Iyer
Death of 18-Year Old Amanda Abbiehl and Opioid-Induced Respiratory Depression: Physician-Patient Alliance for Health & Safety Releases Podcast on Fifth Death Anniversary
In honor of July 17, the day that 18-year old Amanda Abbiehl died five years ago after being connected to a patient-controlled analgesia (PCA), the Physician-Patient Alliance for Health & Safety (PPAHS) has released the podcast, “Opioid-Induced Respiratory Compromise Can Be Prevented”.
The podcast is now available on: Continue reading “Death of 18-Year Old Amanda Abbiehl and Opioid-Induced Respiratory Depression: Physician-Patient Alliance for Health & Safety Releases Podcast on Fifth Death Anniversary”
Preventing Blood Clots in Pregnancy: A Podcast with Maternal/Perinatal Patient Safety Expert Colleen Lee
“Preventing Blood Clots in Pregnancy” – a podcast on the heightened risk of blood clots in pregnant women, the use of simple devices like sequential compression devices to help prevent blood clots, and the role of the OB VTE Safety Recommendations – is now available at the Physician-Patient Alliance For Heath & Safety YouTube channel at http://bit.ly/1He3MLy
On iTunes, the podcast is available at https://itunes.apple.com/ca/podcast/physician-patient-alliance/id897887688?mt=2 Continue reading “Preventing Blood Clots in Pregnancy: A Podcast with Maternal/Perinatal Patient Safety Expert Colleen Lee”
Aspiration and Risks of Anesthesia
By Patricia Iyer MSN RN LNCC
(Pat is a legal nurse consultant who provides education to healthcare providers about patient safety. She can be reached at patriciaiyer@gmail.com)
I woke up from a routine colonoscopy with coughing and not being able to speak. What went wrong?
The gastroenterologist told me I started coughing during the procedure. I inhaled some saliva into my lungs.
Aspiration is the entry of food, liquid, saliva, or stomach contents into the lung. The seriousness of this event can range from minor to a chemical pneumonia to death. Food particles that block the airways can cause suffocation. The people who are at risk for aspiration include people receiving anesthesia, those on ventilators, people with drug overdoses, strokes, traumatic brain injuries, and alcohol intoxication. These individuals have decreased gag reflexes, and are therefore at risk for getting substances into their lungs.
10 Reminders to Ensure Safer Use of Patient-Controlled Analgesia
PCA-related device events are three times as likely to result in injury or death. As Tim Ritter (Senior Patient Safety Analyst, Pennsylvania Patient Safety Authority) reminds us, “Over the six-year period from June 2004 to May 2010, data collected by Pennsylvania Patient Safety Authority revealed that there were approximately 4,500 reports associated with PCA pumps. Moreover, U.S. Food and Drug Administration’s (FDA) Manufacturer and User Device Experience (MAUDE) database demonstrates that PCA-related device events are three times as likely to result in injury or death as reports of device events involving general-purpose infusion pumps.” Continue reading “10 Reminders to Ensure Safer Use of Patient-Controlled Analgesia”
Patient Controlled Analgesia Pumps: 5 Sources of Dangers – Part 2
by Pat Iyer, president of www.avoidmedicalerrors.com and president of Med League at http://www.medleague.com. She reviewed medical surgical nursing liability cases for 20 years.
1. Misprogramming the pump
Many errors can happen when the PCA pump is programmed to deliver the narcotic. A point by point checklist is a helpful safety measure that has not be available until now. Continue reading “Patient Controlled Analgesia Pumps: 5 Sources of Dangers – Part 2”
Sources of Dangers with Patient Controlled Analgesia Pumps (Part 1)
by Pat Iyer, president of www.avoidmedicalerrors.com and president of Med League at http://www.medleague.com. She reviewed medical surgical nursing liability cases for 20 years.
Both physicians and nurses can contribute to errors that harm patients receiving PCA pumps. These pumps are typically used primarily in the hospital for pain control. The premise behind the pumps is that the patient is the best judge of when he or she needs pain medication. Giving the patient control of the pump eliminates the time the patient has to wait for a nursing staff member to bring a pain pill or injection. The theory of the pumps is wonderful; the reality is that they are dangerous if not ordered correctly or their use monitored appropriately.
Continue reading “Sources of Dangers with Patient Controlled Analgesia Pumps (Part 1)”
3 Risks with Managing Pain with Patient-Controlled Analgesia (PCA) Pumps
According to reports made to the Food and Drug Administration (FDA) between 2005 and 2009, more than 56,000 adverse events and 700 patient deaths were linked to infusion pumps. One out of 378 post-surgical patients are harmed or die from errors related to the infusion pumps that help relieve pain after surgical procedures, such as knee or abdominal surgery.
In a recent interview, Pat Iyer, MSN, RN, LNCC, president of avoidmedicalerrors.com, Cindy and Brian Abbiehl of A Promise to Amanda Foundation, and Michael Wong, JD of the Physician-Patient Alliance for Health & Safety discussed patient-controlled analgesia (PCA) pumps and 4 risks when using patient-controlled analgesia (PCA) pumps. Continue reading “3 Risks with Managing Pain with Patient-Controlled Analgesia (PCA) Pumps”
Patient Controlled Analgesia (PCA) Pumps: The Basics
by Pat Iyer, president of www.avoidmedicalerrors.com
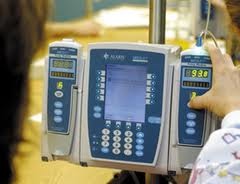
Patient Controlled Analgesia (PCA) pumps were developed to address the problem of undermedication. They are used to permit the patient to self-administer small doses of narcotics (usually Morphine, Dilaudid, Demerol, or Fentanyl) into the blood or spinal fluid at frequent intervals. PCA pumps are commonly used after surgery to provide a more effective method of pain control than periodic injections of narcotics. This method of pain control has been found to result in less pain and earlier discharge from the hospital. PCA pumps can be effectively used by children as young as six years old. A continuous infusion (called a basal rate) of 1-2 mg/hour permits the patient to receive a continuous infusion of pain medication. This mode of delivery is now used only for patients who have had prior opioid use or are not “opioid naïve”. The risk of respiratory depression is too great in patients who have not built up a tolerance to opioids. Typically the patient receives an intravenous “loading” dose to quickly raise the blood level of the pain medication.
Continue reading “Patient Controlled Analgesia (PCA) Pumps: The Basics”

