by Sean Power
February 4, 2014
The Institute for Healthcare Improvement (IHI) held on January 22, 2014 a special webinar for the Perinatal Improvement Community on safety recommendations for maternal patients. You can download the webinar recording and slides here.
The webinar featured Peter Cherouny, MD, Emeritus Professor, Obstetrics, Gynecology, and Reproductive Sciences, University of Vermont, Chair and Lead Faculty of the IHI Perinatal Improvement Community and Michael Wong, JD, Executive Director of the Physician-Patient Alliance for Health and Safety (PPAHS).
Maternal death rate in the USA has more than doubled in the last 25 years and data from the Centers for Disease Control and Prevention (CDC) show that pregnancy-related mortality is rising in the United States.
According to William M. Callaghan, MD, MPH Chief, Maternal and Infant Health Branch Division of Reproductive Health, National Center for Chronic Disease Prevention and Health Promotion, CDC:
“These statistics may represent a conservative estimate of the problem. Why? Not all pregnancy-related deaths are accurately identified and reported. Hence, pregnancy-related deaths identified at the national level likely undercount the true number.”
“The United States is down close to the bottom of the top fifty,” says Mr. Wong when looking at maternal death rate compared by country, with 21 deaths per 100,000 live births in 2010. This ranking is particularly alarming because the U.S. spends more money per capita for maternity care than any other country.
There has been “an eight-fold increase in the maternal age group 35 and older in the last thirty to forty years,” says Dr. Cherouny. “Not surprisingly, just like all of us, as we age, underlying diseases tend to present themselves, particularly related to pregnancy sometimes,” he explains.
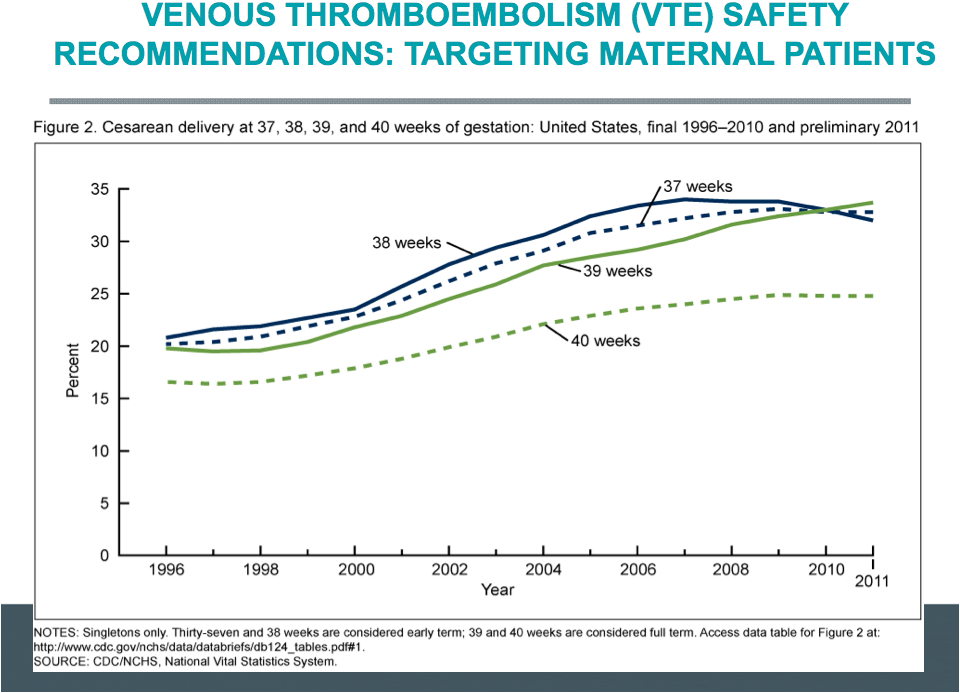
“Of course, an important contributor to that has been the operative delivery rate. We know that has gone up over 50 percent just in the last decade and about 60-65 percent in the last 15 to 18 years,” says Dr. Cherouny. According to Dr. Cherouny, surgical intervention increases the relative risk of thromboembolic phenomenon for obstetric patients, who due to pregnancy, are at a four- to five-fold increased relative risk.
Venous thromboembolism (VTE) costs the health care system more than $1.5 billion per year, according to research in 2009 by Dobesh PP, published in Pharmacotherapy.
The research also found that deep vein thrombosis costs anywhere from $7,712 to $10,804 per patient; pulmonary embolism costs $9,566 to $16,644.
According to Dr. Andra James, Professor of Obstetrics and Gynecology, Division of Maternal Fetal Medicine, University of Virginia School of Medicine:
“For pregnant women, the risk of VTE is 4-5 times higher than women who are not pregnant. Moreover, this risk is at least twice as much following cesarean delivery.”
Pregnancy is a major risk factor for developing venous thrombosis and pulmonary embolism, especially following cesarean delivery, non delivery admissions and up to one month post partum.
The true reason for OB VTE prevention
“One patient is one too many,” says Mr. Wong. “This is the true reason for advocating for OB VTE prevention.”
In 2012, Amber Scott was found unresponsive by her husband. After determining that Amber had a blood clot in her brain, doctors performed an emergency c-section.
“Thankfully a beautiful baby girl was born,” continues Mr. Wong. “But unfortunately, Amber was in a coma.”
Amber came out of the coma many weeks later and is still going through rehabilitation more than a year and a half later.
“In a sense, Amber is the lucky one,” says Mr. Wong. “She survived.”
Amee VanTassell, age 36, “tragically died of a blood clot four days after delivering her baby daughter from c-section,” according to Mr. Wong. Several other patients have been similarly impacted by preventable VTE such as Samara McAuliffe, Lisa Boyd, and Jessica Phillips.
Cesarean delivery a contributing factor to risk for VTE
According to Dr. Cherouny:
“From a gynecologic standpoint, when we look at surgery alone, we know that about literally—this always surprises me when I look at it—in non-prophylactic patients undergoing significant gynecologic surgery, 15 to 40 percent of them develop a DVT [deep vein thrombosis]. So it’s not surprising that the risk factors are there and can be translated to the obstetric community with the increased cesarean surgical rate that we’ve seen.”
Research by Steven L. Clark, MD, et. al. examines the causal relationship between route of delivery and maternal death.
“As Dr. Clark did,” Dr. Cherouny says, “if you back out the venous thromboembolic deaths in these subgroups, we begin to see at the end of it a non-significant difference both between vaginal and primary cesarean section and between vaginal and repeat cesarean section.”
Continues Dr. Cherouny, “overall the data pool showed a non-significant difference between route of delivery and maternal death when you excluded pulmonary embolism.”
“In other words,” Dr. Cherouny explains, “if we were perfect in our prevention for venous thromboembolism and pulmonary embolism, we may see a dramatically different overall risk association, particularly with our operative deliveries.” This is clinically significant.
Every year about 4 million deliveries occur across the U.S. Approximately 33.7 percent of these deliveries occur as cesarean sections, equal to 1.34 million cesarean sections occurring every year. According to Dr. Cherouny, considering that scale even low incidence outcomes become important.
According to Dr. Cherouny:
“Essentially every patient is at moderate risk. The only exceptions to that would be patients who have surgery less than 30 minutes who are under 40 who have no other risk factors. I would make the argument that no patients are low risk.”
As Dr. Cherouny explains, even though some cesarean surgeries are performed in less than 30 minutes, the VTE risk clock starts during induction of anesthesia.
“If you take that into account,” Dr. Cherouny says, “there is really no case of a patient in the low risk category undergoing a cesarean section.”
Effective risk assessment for VTE begins with pneumatic compression devices
“For effective risk assessment to occur, you’re really trying to put patients in different risk categories,” says Dr. Cherouny. “Effective risk prophylaxis assessment is going to lead to appropriate risk-based therapy.”
Because the vast majority of patients undergoing operative delivery are at moderate or high risk for VTE, Dr. Cherouny says that it is important for providers to take the necessary steps to prevent VTE from taking place.
Dr. Cherouny states:
“All patients having a cesarean delivery should have pneumatic compression devices placed prior to surgery.”
Pneumatic compression is a therapeutic technique that uses devices such as an inflatable sleeve around an extremity requiring treatment to pressurize tissues and the venous system in the extremity. By enhancing blood flow/venous return, pneumatic compression reduces the chance that deep vein blood clots form. By preventing deep venous thrombosis, pneumatic compression devices help prevent VTE and related adverse events and sequale.
OB VTE Safety Recommendations
The PPAHS, in collaboration with the IHI and the National Perinatal Association, announced in December the compilation of VTE safety recommendations.
The recommendations, compiled by a panel of health experts, give providers a step-by-step checklist to help assess all OB patient’s risk for VTE and identify the appropriate prophylaxis regimen to improve health outcomes for maternal patients.
You can download a checkable version of the OB VTE Safety Recommendations Checklist here.