By Sean Power
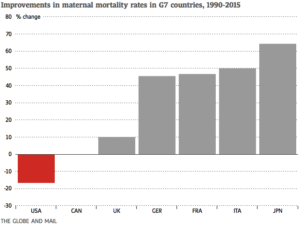
An article by The Globe and Mail highlights a World Health Organization (WHO) report showing that the United States is falling behind Canada when it comes to maternal mortality.
According to the WHO report, the US average declined to 14 maternal deaths per 100,000 live births in 2015; Canada’s figure sits at 7, where it was in 1990.
According to the report, maternal mortality fell worldwide by 43 percent during the 25-year period. The decrease can be attributed to better access to improved health services during and after pregnancy and childbirth, as well as better sexual and reproductive health services and family planning.
The world average is 216 deaths per 100,000 live births. In rich countries, the average is lowest among rich countries (12) and highest in sub-Saharan Africa (546).
The US joins North Korea, South Africa, Venezuela, the Bahamas, Georgia, Serbia, Guyana, Jamaica, Saint Lucia, Suriname, Tonga, and Zimbabwe as the world’s only countries where maternal mortality has worsened between 1990 and 2015.
This trend is particularly alarming when one considers that the US spends more money per capita for maternity care than any other country.
Source: Centers for Disease Control and Prevention
Drivers of Maternal Mortality in the United States
The Physician-Patient Alliance for Health & Safety (PPAHS) prioritizes maternity care as a patient safety priority, specifically with respect to venous thromboembolism (VTE) among maternal patients.
According to Peter Cherouny, MD, Emeritus Professor, Obstetrics, Gynecology, and Reproductive Sciences, University of Vermont, Chair and Lead Faculty of the Institute for Healthcare Improvement (IHI) Perinatal Improvement Community, there has been an eight-fold increase in the maternal age group 35 and older in the last thirty to forty years. The operative delivery rate has increased over 50 percent in the past ten years and about 60-65 percent in the last 15 to 18 years, and surgical intervention increases the relative risk of VTE for obstetric patients, who, due to pregnancy, are already at a four- to five-fold increased relative risk of VTE.
Pregnancy is a major risk factor for developing VTE, especially following cesarean delivery, non-delivery admissions, and up to one-month post partum.
According to Dr. Andra James, Professor of Obstetrics and Gynecology, Division of Maternal Fetal Medicine, University of Virginia School of Medicine:
“For pregnant women, the risk of VTE is 4-5 times higher than women who are not pregnant. Moreover, this risk is at least twice as much following cesarean delivery.”
These factors heighten the risk of serious adverse events including death among maternal patients.
According to Dr. Cherouny:
“From a gynecologic standpoint, when we look at surgery alone, we know that about literally—this always surprises me when I look at it—in non-prophylactic patients undergoing significant gynecologic surgery, 15 to 40 percent of them develop a DVT [deep vein thrombosis]. So it’s not surprising that the risk factors are there and can be translated to the obstetric community with the increased cesarean surgical rate that we’ve seen.
“As Dr. Clark did [Steven L. Clark, MD, et. al.], if you back out the venous thromboembolic deaths in these subgroups, we begin to see at the end of it a non-significant difference both between vaginal and primary cesarean section and between vaginal and repeat cesarean section.
“Overall the data pool showed a non-significant difference between route of delivery and maternal death when you excluded pulmonary embolism.
“In other words, if we were perfect in our prevention for venous thromboembolism and pulmonary embolism, we may see a dramatically different overall risk association, particularly with our operative deliveries.”
Given Dr. Cherouny’s statement that if we perfect our prevention for VTE then risk association could be significantly different, could a focus on OB VTE reverse the troubling trend in maternal mortality?
PPAHS, in collaboration with the IHI and the National Perinatal Association made available OB VTE Safety Recommendations.
Download the OB VTE Safety Recommendations here.
Canada and the United States are similar in many respects from a socioeconomic standpoint. Why do you think Canada has outperformed the USA in the area of maternal mortality? Leave a comment below.